Antisynthetase Syndrome (AS)
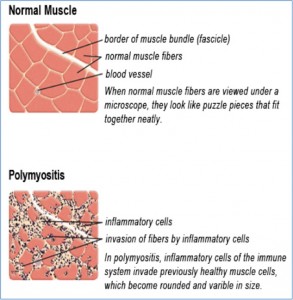
Antisynthetase syndrome (AS), one of the inflammatory myopathies, is sometimes called Anti-Jo1 syndrome or AS syndrome and is an autoimmune condition characterized by having autoantibodies to aminoacyl transfer RNA synthetases (anti-ARS) and includes a collection of symptoms/clinical features (syndrome) including myositis, polyarthralgia, Raynaud’s phenomenon, Mechanic’s hands, unexplained fevers, and interstitial lung disease (ILD).
Not all clinical features will be present in every patient. Each patient is unique. Learn more about diagnosing and treating antisynthetase syndrome below.
Antisynthetase syndrome criteria
Not all have to be present
The presence of an antisynthetase antibody) plus two major or one major and two minor criteria is required for a diagnosis of antisynthetase syndrome according to criteria by Solomon et al (2011):
Major Criteria
- Interstitial lung disease (ILD)
- Polymyositis (PM) or Dermatomyositis (DM)
Minor Criteria
- Polyarthritis (inflammation of many joints)
- Raynaud’s Phenomenon
- Mechanic’s Hands
Other symptoms and complications
Other symptoms, do not occur in all patients.
- Unexplained Fevers
- Loss of appetite
- Weight loss
- Fatigue (can be extreme and life-altering)
- Symptoms and complications of polymyositis or dermatomyositis such as muscle weakness, muscle pain, and skin rashes.
Who is affected by Antisynthetase syndrome?
Antisynthetase syndrome (AS) is a rare disease. A rare disease in the U.S. is defined as a condition affecting fewer than 200,000 people.
Here is some additional information:
- Antisynthetase syndrome affects twice as many women as men.
- The average age of antisynthetase syndrome onset is 50.
- Interstitial lung disease may be the first and only symptom of antisynthetase syndrome for some.
- The risk of mortality increases when there is severe and extensive interstitial lung disease (ILD).
An accurate and expeditious diagnosis is vital for proper treatment, especially when there is lung involvement. Seeing a doctor with experience is highly recommended.
Pain and Antisynthetase syndrome
Myalgia (muscle pain) is a reality for many patients with myositis and this includes those with antisynthetase syndrome.
Pain may also be present with arthritis.
Antisynthetase Antibodies
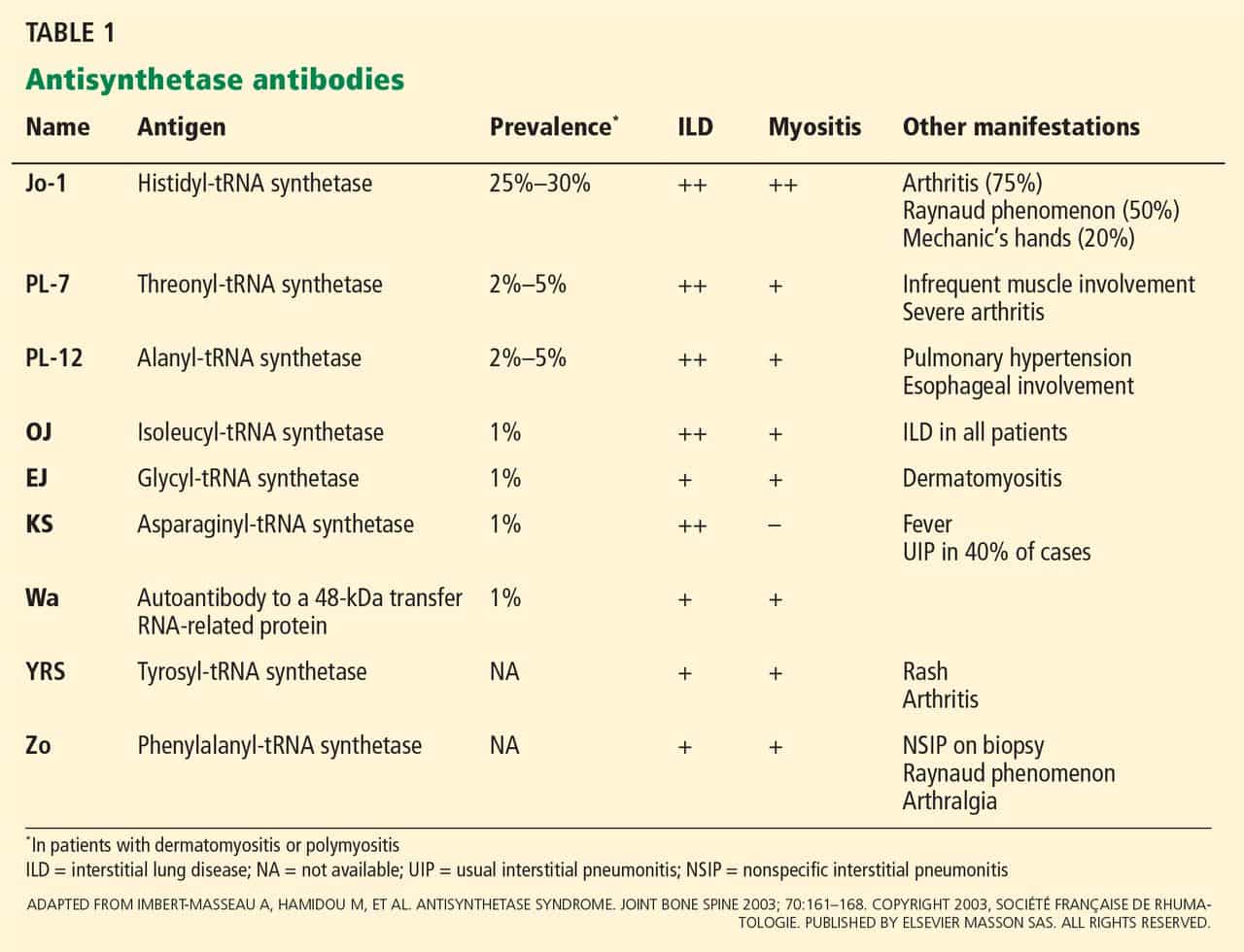
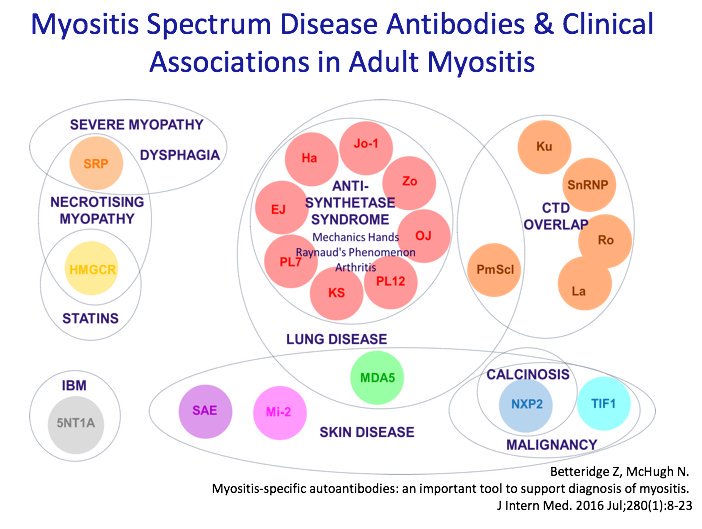
Antisynthetase syndrome is associated with a number of known autoantibodies called aminoacyl-tRNA synthase (ARS) autoantibodies.
Anti-Jo-1, anti-PL-7, anti-PL-12, anti-EJ, anti-KS, anti-OJ, anti-Ha, and anti-Zo antibodies target aminoacyl-tRNA synthetases and represent antisynthetase syndrome.
Anti-Jo-1 is the most common autoantibody seen in antisynthetase syndrome and is present in an estimated 70-90% of patients with Myositis who have associated Interstitial Lung Disease.
Other autoantibodies are also seen with antisynthetase syndrome, however, these autoantibodies constitute a small percentage of Myositis/Interstitial Lung Disease patients.
Breaking it down further
Symptoms may correlate with autoantibodies. Remember, this does not mean each patient will have the same symptoms as noted below.
- Anti-Jo-1: myopathy, severe arthritis, and mechanic’s hands.
- Anti-PL-12: higher rates of Raynaud’s phenomenon
- Anti-PL-7, anti-PL-12, anti-KS, and anti-OJ: cases of ILD
- Anti-PL-7: presence of heliotrope rash
Diagnosing Antisynthetase syndrome
Which doctors do I see?
Antisynthetase syndrome can be a difficult disease to diagnose and manage. A diagnosis may be suspected based on certain characteristic symptoms and once other diseases have been ruled out. Some patients may be diagnosed by a rheumatologist or neurologist, while others who present with predominant lung disease may be diagnosed by a pulmonologist.
Consultation with other specialists often depends on symptoms, coexisting illnesses, and other organ involvement and may include a dermatologist, cardiologist, oncologist, and a pain management specialist.
Exercise is important for myositis patients. Therefore, you may also see a physical therapist, occupational therapist, and, if you have trouble swallowing (dysphagia), you may also see a speech-language pathologist.
Clinical and Physical Exam
A complete medical and family history is important in helping to diagnosis a rare and complex syndrome. We suggest writing a detailed medical and family history that you can share with your medical team and that can be used for all future appointments.
Blood Testing
Your doctor will likely order various blood tests when suspecting antisynthetase syndrome and may include:
- Various autoimmune, inflammatory, and cancer markers
- Myositis-specific antibodies (MSA)
- Myositis-associated antibodies (MAA)
- Creatine Kinase (CK or CPK) (muscle enzymes)
- Aldolase
- ALT and AST
- LD (Lactate dehydrogenase)
- Sed Rate (also called ESR or Erythrocyte sedimentation rate)
- ANA (Antinuclear Antibodies panel) and other antibodies
High Capacity CT Scan (computed tomography) and Chest X-ray
When lung involvement is suspected, a chest X-ray and High Capacity CT scan of the lungs can help diagnose and check the severity of interstitial lung disease (ILD).
Pulmonary Function Tests (PFT’s)
When the lungs are involved, your physician may order PFTs, a group of tests that measure how well your lungs work. This includes how well you are able to breathe and how effective your lungs are able to bring oxygen to the rest of your body.
EMG and Nerve Conduction Study (NCS)
An EMG (Electromyography) is a test that checks the health of the muscles and the nerves that control the muscles. EMG testing can help distinguish between weakness due to muscle disease from weakness due to nerve problems. Nerve conduction study is usually done during the same visit and is a test to see how fast electrical signals move through a nerve.
MRI (Magnetic Resonance Imaging)
MRI is being used more frequently for myositis and can show changes suggesting muscle inflammation. Physicians may also use MRI to choose the best muscle for biopsy.
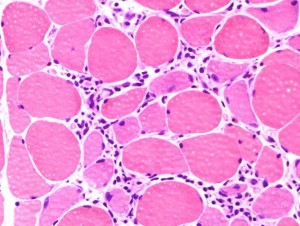
Muscle Biopsy
The muscle biopsy has long been considered a gold standard for a diagnosis of myositis. With autoantibodies and imaging studies, a muscle biopsy may not be necessary. If it is, a doctor will remove a small piece of muscle tissue, usually through an open surgical biopsy, and send it to a lab for testing.
Your doctor will try and choose the weakest muscle, careful to avoid the site of any recent EMG, for biopsy. An MRI can be helpful in locating the best muscle to biopsy.
Lung Biopsy
A lung biopsy may be done to determine more about interstitial lung disease. Learn more about how the lung biopsy procedure is done.
Other Testing
The above tests are not an exhaustive list your physician may use. Other testing will depend upon your symptoms and coexisting illnesses. Some examples are below.
Cancer Screenings
Since some small studies show there may be a slight risk of cancer your doctor may perform several cancer screenings, including those that are age and gender appropriate.
Swallowing Evaluation and Studies
If you have difficulty swallowing (dysphagia) your doctor will likely order testing to determine the source and severity. Dysphagia can be a serious issue and can cause choking and aspiration. There are various diagnostic tests that your doctor may order.
More about dysphagiaChallenges of diagnosing Antisynthetase syndrome
Diagnosing antisynthetase syndrome can be a long and difficult process for several reasons.
- Antisynthetase syndrome is a rare disease. Rare diseases are often more difficult to diagnose. The saying, “When you hear hoofbeats, look for horses, not zebras” is something doctors learn and in many cases works well. The “horses” represent more common diseases and the “zebras” refer to rare diseases, like myositis.
- Each patient with antisynthetase syndrome is unique in how their disease presents and with which symptoms and complications they may have.
- Joint involvement may mimic or even overlap with rheumatoid arthritis.
- Antisynthetase syndrome may appear with or without a rash.
- When interstitial lung disease is the first or only finding, physicians will need to determine if it is primary ILD or if it is a part of antisynthetase syndrome.
Antisynthetase syndrome can mimic other diseases such as primary ILD, primary polymyositis or dermatomyositis, etc.
Antisynthetase syndrome in photos
Treating Antisynthetase syndrome
Treatment goals include reducing muscle, lung, and/or skin inflammation and improving quality of life. Finding a combination of medications and therapies is often necessary for successful results.
Corticosteroids
The initial treatment is typically corticosteroids such as prednisone or prednisolone and may be dosed by the patient’s weight at 1 mg per kg. Corticosteroids address inflammation and simultaneously help suppress the overactive immune system. For severe cases, intravenous methylprednisolone (IV steroids) may be used.
Steroids have many side effects including weight gain and redistribution of body fat to the face, neck, and abdomen; elevated blood sugars, mood swings, thinning of the skin, cataracts, and osteoporosis.
Depending on symptoms, additional drugs to suppress the immune system may be added to the steroids.
Immunosuppressive Drugs
Steroid-sparing agents, such as immunosuppressive drugs and Disease-Modifying Antirheumatic Drugs (DMARDs), have an added benefit as they may help to reduce or eliminate the need for steroids. However, these medications are not without their own risks.
Doctors may use immunosuppressive drugs for patients with antisynthetase syndrome especially in those with severe muscle weakness and interstitial lung disease.
Other Treatments
Rituximab (Rituxan)
Based on research, Rituximab is a good treatment option for those with interstitial lung disease who do not respond well to other treatments. Rituximab belongs to a class of drugs called monoclonal antibodies. It is given intravenously (IV).
See more information about the medications and other treatments by visiting our Treating Myositis page.
Living with Antisynthetase syndrome
Day-to-day management of antisynthetase syndrome can take many forms. Adapting to a “new normal” can be challenging and require many lifestyle changes.
Exercise Program
It was once thought exercise was not good for myositis patients and may cause muscle damage. This has now been proven false through research.
We now know there are massive benefits in having an approved exercise program. This may start with a doctors referral to physical therapy or a rehabilitation center. Exercise plans that are supervised by your medical and healthcare team are most effective so you do not injure yourself.
Before starting any type of exercise plan, talk to your doctor first.
Oxygen Use
Patients may require the use of oxygen due to interstitial lung disease (ILD). This is very helpful but can be a life-changing addition to a patients life.
Diet and Nutrition
Eating a well-balanced diet high in protein may be beneficial for those with myositis, and is for your overall health.
Corticosteroids have many side effects including weight gain and redistribution of body fat to the face, neck, and abdomen, elevated blood sugars, and osteoporosis, so you may need to make adjustments in your diet for these conditions.
Ask your doctor about nutrition and a referral to a dietician or nutritionist.
Support
When living with antisynthetase syndrome, having a good support system in place is extremely helpful.
Antisynthetase syndrome is a chronic illness and some people in your life may not understand the disabling aspects of the symptoms, treatments, and stress involved in managing this complex, sometimes even invisible illness.
We offer several online support options for patients, family members, caregivers, and friends of those living with antisynthetase syndrome. Having an emotional outlet is helpful, and our groups are also educational and resourceful. We, at times, try to add some fun activities aimed at helping reduce stress and get to know one another better.
Antisynthetase syndrome Prognosis
The prognosis of antisynthetase syndrome depends on many varying factors including:
- Symptoms and their severity
- Response to treatment
- Age of onset
- Presence and severity of interstitial lung disease
- Antibodies involved
The following factors may indicate a worse prognosis:
- Age of onset at 60-plus years
- Delayed diagnosis and treatment
- Severe and extensive lung involvement (may necessitate the need for lung transplantation)
- Pulmonary hypertension
- Presence of cancer
- Negative for Jo1 antibody
- Several studies have shown patients that are positive for non-Jo1 antibodies have worse survival rates than Jo1 patients.
Long-term steroid use may also be a major source of morbidity.
Have you been diagnosed with Antisynthetase syndrome?
Get the support you deserve. Join the Myositis Support Community.
Safe, private myositis community for patients and caregivers.
Antisynthetase syndrome In Focus
What does Antisynthetase syndrome look like?
Patients with antisynthetase syndrome may require the use of devices to assist with mobility such as a cane, walker, or wheelchair, either for short periods like during flares or for long-term muscle weakness and damage. When the lungs are involved, some may wear oxygen. Some may look perfectly healthy on the outside, but on the inside, they are very sick and struggling on many levels.
Antisynthetase syndrome resources and education
Below you will find links to resources for research and education.
- Syndrome in question: antisynthetase syndrome (anti-PL-7)
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5087238/ - The Diagnosis and Treatment of Antisynthetase Syndrome
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5006392/ - Clinical manifestations of anti-synthetase syndrome positive for anti-alanyl-tRNA synthetase (anti-PL12) antibodies: a retrospective study of 17 cases
https://academic.oup.com/rheumatology/article/49/5/972/1786211
Research and Clinical Trials
Research helps us better understand diseases and can lead to advances in diagnosis and treatment. Patients are encouraged to look at and participate in clinical trials.
We have partnered with Antidote Technologies to help make your clinical trial match easier. Click the start button below to begin.
Simply Put
“Simply Put” is a service of Myositis Support and Understanding, to provide overviews of Myositis-related medical and scientific information in understandable language.
MSU volunteers, who have no medical background, read and analyze often-complicated medical information and present it in more simplified terms so that readers have a starting point for further investigation and consultation with healthcare providers. The information provided is not meant to be medical advice of any type and is in no way intended to replace professional medical care by a qualified specialist and should not be used as a basis for diagnosis or treatment.
Some images courtesy of The Muscular Dystrophy Association.