Juvenile Myositis (JM)
Juvenile dermatomyositis (JDM) is a systemic, autoimmune inflammatory muscle disorder and vasculopathy that affects children younger than 18 years. JDM primarily affects the skin and the skeletal muscles.
Characteristic findings include Gottron’s papules, a heliotrope rash, calcinosis cutis, and symmetrical, proximal muscle weakness.
Juvenile Myositis (JM), including Juvenile Dermatomyositis (JDM) and Juvenile Polymyositis (JPM), are rare autoimmune conditions which cause inflammation. The inflammation for JPM primarily occurs in the muscles, while in JDM the inflammation is in the blood vessels that lie under the skin and in the muscle tissue. This inflammation causes weak muscles and – in the case of JDM – skin rashes. If blood vessels or muscle cells in other parts of the body are inflamed, other systems of the body can be affected, such as the digestive tract, heart, and lungs. The condition itself and the treatment for the disease can be life-threatening.
The cause of the autoimmune response causing JM is thought to be a result of several factors, both environmental and genetic. Children who develop this disease often have a family history of other autoimmune diseases, such as thyroid disorder, type I diabetes, rheumatoid arthritis, lupus, or Crohn’s disease. If a child is genetically predisposed to JM, experts suspect a microbe, such as a virus or bacteria, may trigger an overactive immune response that can cause the body to attack itself.
While the exact incidence is unknown, estimates from various studies suggest that between 1 and 5 children per million will develop this disease each year. Approximately 1,000 new cases of JM are diagnosed in the United States every year, and 22,000 annually worldwide.
The average age of onset for JDM is between six to seven years old, while JPM usually develops several years later. JM affects girls twice as much as boys. Once a child is diagnosed with JM, it is always considered to be the juvenile form, even if the patient continues with the disease into adulthood.
There is no cure for JM, but with advances in early diagnosis and aggressive treatment, the outcome has continued to improve. Some children experience a mild form of the disease and may go into remission. Others follow a more severe and potentially debilitating course that can cause a life-long struggle. Some JM patients will have a loss of range of motion. Some will battle an array of serious complications, resulting in the inability to walk, ongoing pain, disfigurement, and even death. Whether the course of the disease is mild or severe, JM is life-changing for all of these children and their families.
Skin involvement of Dermatomyositis can precede or accompany weakening muscles, primarily in the core of the body such as the stomach, thighs, neck, and upper arms. Other muscles, however, can become weak as well. Sometimes there is inflammation in the swallowing muscles or esophagus, which makes it difficult for the child to swallow. Other times, there is inflammation in the intestinal tract, which may cause bowel difficulties and stomach pain.
A child with JM has great difficulty climbing stairs and just getting up from a sitting position. Walking and running become very challenging and exhausting. Some children will literally roll out of bed, because sitting up and lifting the head becomes too difficult. In addition to weakness, some children with JM experience muscle pain.
Interesting Facts:
JM is a rare disease and its exact incidence is unknown. Approximately 2 to 4 children in a million in the United States are diagnosed with JM each year.
JM begins in childhood or the teen years. The average age of onset for JDM is between six to seven years old; 25% are age 4 or less. JPM usually develops several years later.
JM affects girls twice as much as boys. Once a child is diagnosed with JM, it is always considered to be the juvenile form, even if the patient continues with the disease into adulthood. Cure JM
Signs, Symptoms, and Complications of Juvenile Myositis
Skin Rashes
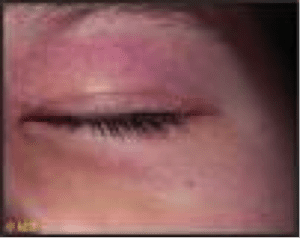
The skin rash in JDM usually occurs on the eyelids, knuckles, elbows, knees, and ankles. The rash may appear before, after or at the same time as the muscle weakness. Sometimes the rash is so faint that it is not noticeable.
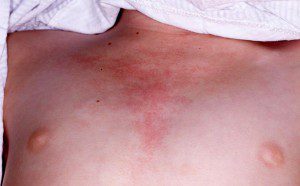
A rash appearing on the eyelids is red and purplish in color and is referred to as a heliotrope rash (named after a flower of the same color). Another rash that frequently occurs on the cheeks takes on a red color and looks very similar to sunburn.
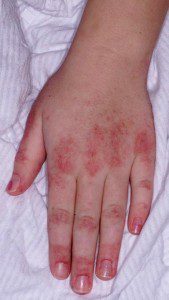
On the knuckles, elbows, and knees, the rash takes the form of patches of red and scaly skin (called Gottron’s papules). The fingernails and the nail beds may take on a pinkish color as well.
JM affects every child differently. Some children experience a mild form of the disease, while others follow a more severe and potentially more debilitating course. Some of the more onerous secondary symptoms are calcinosis, digestive (GI) tract complications, vasculitic ulcers, and contractures.
Fatigue
With JM, the child becomes tired easily and can only walk short distances. The child needs to rest often and lacks the energy for normal activities. It becomes difficult for the child to keep up with friends.
Digestive Issues
The Gastrointestinal (GI) tract refers to the digestive system including the esophagus (swallowing tube), stomach and intestines. Myositis can cause the muscles in the GI tract to become inflamed and they may not be strong enough to move food through the digestive tract. Symptoms of GI tract problems include:
Because the major problem in JDM is a systemic vasculopathy, which means that small blood vessels are damaged, the absorption of medication and nutrition from the gastrointestinal tract may be impaired. Doctors may sometimes offer alternative treatments, such as IV medications, IV nutrition or a feeding tube, to ensure that the medication and nutrition is properly absorbed. In some cases, a nutritionist or speech pathologist may also be consulted.
Sometimes, GI issues are also a side effect of the medications used to treat juvenile myositis. GI complications can be serious. Alert your medical team right away if your child experiences any GI issues, in particular: Severe abdominal pain or pain that becomes progressively worse. Blood in the stool or dark, sticky stool. In some cases, this could indicate vasculitic ulcers in the intestines, which can be a serious complication of myositis.
Fever and/or Irritability
Sometimes, the child with JM runs low-grade fevers, especially at night. You may notice your child seems quite irritable and their behavior may become more difficult than normal.
Calcinosis
Researchers believe approximately 10% to 50% of the children with JM will develop calcinosis. Calcinosis is the development of small lumps or linear deposits of calcium under the skin or in the muscle. They may feel like rocks under the skin and can range in size from a small pebble to a large softball. They can also form in a sheet-like appearance. In many cases, these calcium deposits can grow over time or remain unchanged for years. In some cases, calcinosis lumps are absorbed back into the body. Other times, the lumps break through the skin where they may leak creamy white calcium. These protrusions can become infected and painful, and sometimes need to be surgically removed. Calcinosis lumps are most likely to break through on the joints, such as the elbows and knees, but they can emerge anywhere on the body, often in pressure points. Calcinosis can be present at the time of diagnosis, or many years later. It can be associated with a delayed diagnosis or the lack of aggressive treatment.
Vasculitic Ulcers
Vasculitic ulcers are holes in the skin or gastrointestinal tract caused by inflammation of the blood vessels. When they occur in the skin, they look like open sores and can extend deep into the tissues. The ulcers can be very painful and generally are associated with a more severe course of JM. When the ulcers occur in the gastrointestinal tract, they can harm the digestive organs and result in very serious illness. The warning signs of this condition are severe stomach pain, dark black stools or blood in the stools.
Contractures
Contractures are shortened muscles that cause a joint to stay in a bent position or have limited movement. Contractures can occur due to inflammation, muscle weakness, or calcinosis crossing over a joint.
Lipodystrophy
Lipodystrophy is a loss of body fat. In areas affected by lipodystrophy, the fat cells become damaged, and if widespread and extensive, this can result in problems with storing fat and sugar, resulting in high cholesterol and diabetes.
Diagnosing Juvenile Myositis
A doctor will first perform a complete physical exam, specifically looking for rashes and muscle weakness.
If JM is suspected, blood tests are the next step in making a diagnosis. Muscle enzymes are measured, including creatine kinase (CK or CPK), aldolase, lactate dehydrogenase (LDH), aspartate aminotransferase (AST) and alanine aminotransferase (ALT). If these lab tests are elevated, enzymes are leaking from inflamed or damaged muscles into the bloodstream.
Antinuclear antibodies (ANA) are also measured to see if the child’s body is producing antibodies against its own cells. Several myositis-specific autoantibodies have also been identified, and these can be tested as well. Other blood tests are sometimes available to check out immune activation and/or blood vessel damage.
The next step in diagnosing JM is usually an MRI, which can detect muscle inflammation and damage. If the MRI shows evidence of diseased muscles, a muscle biopsy may be performed to finalize the diagnosis. When the characteristic rashes are not present, it is important that a muscle biopsy be performed to exclude other causes of muscle weakness. A small amount of muscle is removed for examination under a microscope to determine if and how much the muscles and blood vessels have been affected by the disease.
Simply Put
“Simply Put” is a service of Myositis Support and Understanding, to provide overviews of Myositis-related medical and scientific information in understandable language.
MSU volunteers, who have no medical background, read and analyze often-complicated medical information and present it in more simplified terms so that readers have a starting point for further investigation and consultation with healthcare providers. The information provided is not meant to be medical advice of any type.
Cure JM Foundation™
Cure JM Foundation™ is a 501(c)(3) nonprofit organization dedicated to finding a cure for Juvenile Dermatomyositis (JDM) and Juvenile Polymyositis (JPM), the rare and life-threatening autoimmune diseases collectively known as Juvenile Myositis (JM). Approximately 2 to 4 children in a million in the United States are diagnosed with JM each year.