Myositis: The Basics
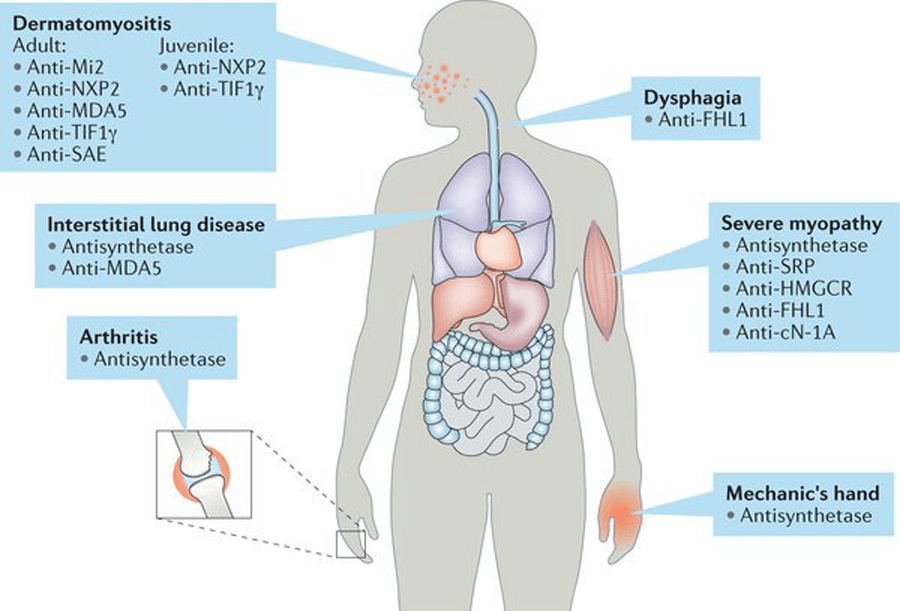
The Idiopathic Inflammatory Myopathies (IIM), which are generally referred to as Myositis, is a group of rare, acquired (not inherited), incurable, systemic autoimmune diseases. While myositis is classified as a muscle disease, it can also affect the heart, lungs, skin, and GI tract, and can be associated with cancer.
IIMs are thought to be caused by an overactive immune system that has gone haywire and attacks the body’s own muscles, connective tissue, blood vessels, skin, lungs, and other organs. Idiopathic means the cause is unknown.
The IIMs are highly variable diseases. Two patients with the same diagnosis can present differently, test differently, and respond to available off-label treatments differently.
There is only one FDA approved therapy for any form of Myositis.
Idiopathic Inflammatory Myopathy (IIM)
May include myositis:
Other forms:
Check out Myositis Videos
Check out our growing library of videos to learn more about the various types of Myositis, and with topics such as clinical trials, exercise, mental health, caregiving, and patient opportunities to get involved.
What Does Myositis Mean?
The prefix ”myo” means muscle and the suffix “itis” means inflammation. Therefore, Myositis is inflammation of the muscle. The term “myopathy” indicates any disease of muscle, whereas “Myositis” is a specific group of muscle diseases, in our case, the idiopatic inflammatory myopathies, which are most often both idiopathic (no known cause) and thought to be autoimmune in nature.
We have found through experiences shared in our Support Groups that some people are diagnosed with “Myalgia and Myositis,” which is actually not a Myositis disease diagnosis, but rather symptoms. The terms simply mean that the patient is experiencing muscle weakness and pain, which can be indications of many diseases, including IIM. However, this diagnosis on its own is not the “Myositis” we discuss as IIMs.
How Does Myositis Affect People?
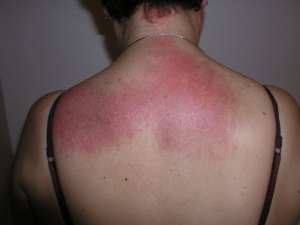
Myositis, such as Poly- and Dermato-, is a rare, chronic, progressive, inflammatory disease which most often is indicated by symmetrical proximal muscle weakness and skin rashes, and for some, chronic pain. Other symptoms may include fatigue (or asthenia), trouble swallowing, shortness of breath, lung disease, fevers, and weight loss. Patients often have difficulty climbing stairs, rising from a seated position, turning over in bed, raising their arms over their head, and may become prone to falls. Symptoms can appear gradually, over a period of months or even years, or they may develop more rapidly, within days or weeks.
With Inclusion Body Myositis (IBM), the muscle weakness may be asymmetric and involves the distal muscles. The weakness is often slow and progressive. Inclusion Body Myositis is the most common type of acquired myopathy in patients over the age of 50. First signs may be frequent falls and difficulty with pinching (affects the finger flexors). With IBM, patients are at risk of dysphagia (trouble swallowing) leading to the potential of choking and aspiration pneumonia.
Depending upon the amount of muscle weakness and extent of muscle wasting, some patients may require the use of a cane, walker, wheelchair, power chair, or other assistive devices. Some may also require the use of toilet lifts such as LiftSeat.
Pinterest Assistive Devices Board
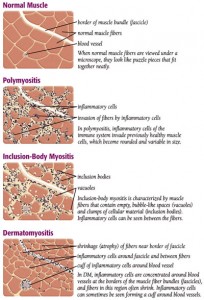
The Inflammatory Myopathies
The Inflammatory Myopathies are a group of rare diseases that involve chronic muscle inflammation, muscle weakness, and, in some cases, muscle pain. These include Dermatomyositis, Clinically Amyopathic Dermatomyositis, Antisynthetase Syndrome, Polymyositis, Inclusion Body Myositis, the Juvenile forms of Polymyositis and Dermatomyositis, and Immune-Mediated Necrotizing Myopathy.
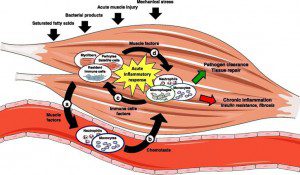
What Causes Myositis?
While there are some known causes of Myositis such as medications, toxins, infections, electrolyte level imbalance, trauma, and thyroid and inherited diseases, many doctors and researchers believe the majority of Myositis (the Idiopathic Inflammatory Myopathies) cases are caused by a misguided immune system response leading to an autoimmune response. The immune system normally fights infections, but for often unknown reasons in autoimmune diseases, the immune system wages an attack on the body’s own normal, healthy tissues.
Does Myositis Cause Pain?
The short answer is yes, for some patients Myositis does cause pain. According to the latest statistics, about 40% of U.S. Myositis patients experience pain.
Doctors were taught in medical school for many years that pain was not associated with Myositis and some doctors may still believe this. The doctors that truly know Myositis, however, will tell you that pain can be a part of Myositis and can be debilitating. We were advised by a leading Myositis specialist and researcher that 50% of her Myositis patients experience pain.
Is Myositis A Rare Disease?
According to the National Organization for Rare Disorders (NORD), the IIMs and subtypes are rare diseases. It is currently estimated that 5-10 people per million are diagnosed with a type of Myositis each year. In the U.S., that equates to only 1,600 to 3,200 cases per year. The exact number of Myositis cases is difficult to measure, but according to the latest estimate, it was thought, with all forms combined, that there are 50,000 to 75,000 people living with Myositis in the U.S.
Who Gets Myositis?
Although Myositis can affect people of any age, most children who get the disease are between 5 and 15 years of age and most adults are between 40 and 60 years of age. Like many autoimmune diseases, most types of Myositis affect more women than men with the exception being Inclusion Body Myositis, which affects more men than women.
How Is Myositis Diagnosed?
Diagnosing Myositis can be a lengthy and challenging process, taking years for some to be officially diagnosed. The symptoms can resemble other, more common diseases and each patient presents differently. Additionally, since most medical professionals lack experience with Myositis, it is not uncommon for patients to be misdiagnosed, which may require seeing multiple specialists prior to receiving an accurate diagnosis and starting a treatment plan.
There are a variety of comprehensive tests which are frequently used in a differential diagnosis, which helps eliminate other possible diseases and pinpoint a more accurate diagnosis. This is not an exhaustive listing, but rather some of the common testing.
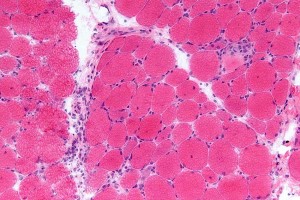
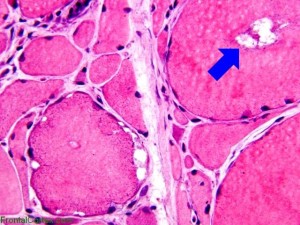
Muscle biopsies used to be considered the best way to determine a diagnosis. However, with Myositis antibodies, MRI, and other less invasive testing, muscle biopsies may not be necessary. This is especially true with Dermatomyositis when findings are “typical.”
Diagnosing MyositisType Of Doctors You May See
Myositis is a systemic disease often affecting more than just the muscles. Therefore, you may see various specialists over time depending on the systems involved. Here are just some of the specialists you may see, usually in coordination with a primary care physician (PCP):
See Tips for finding a Myositis specialist.
Find Myositis SpecialistsCan Myositis Be Cured or Treated?
There is currently no cure for any form of Myositis, however, with proper, expeditious treatment, some patients may experience partial or complete remission, or as we like to call it disease stability. Others may experience active or progressive disease of some or all symptoms for their entire lives. The exception is Inclusion Body Myositis (IBM). There are currently no treatment options available for IBM thus remission is not currently an option.
What Types Of Treatments Are Effective For Myositis?
While no medications have been developed specifically to treat Myositis, several medications and therapies used to treat other autoimmune and inflammatory diseases have been shown to be effective in treating the symptoms in many patients. For the types of Myositis which respond to treatment, corticosteroids, such as Prednisone, are typically the initial treatment followed by immunosuppressive agents. It is not uncommon for patients to try multiple medications, sometimes in combination with infusions, to find the right treatment combination for each individual.
Myositis affects each patient differently often making treatment a trial-and-error process. Finding the right medication or combination of medications is important to help slow the autoimmune process. If left untreated, Myositis can cause significant morbidity and even death.
Exercise is an important part of treating Myositis. It was once thought that exercise would cause more damage to the muscles but this has since been proven false. Talk to your doctor about starting an exercise program.
There are also refractory cases in which patients do not respond to the typical medications used in treating Myositis.
Inclusion Body Myositis does not currently have any treatment options aside from exercise, which is often recommended for all myositis patients now. However, there are ongoing clinical trials for IBM and other forms of Myositis.
Clinical Trials For Myositis
There are ongoing clinical trials for many forms of Myositis. Rare disease patients can be difficult to recruit for trials. We hope you will consider taking a look at clinical trials that may be relevant to you and learn more about getting involved in these important studies.
Search Myositis Clinical TrialsAbout MSU
Myositis Support and Understanding Association (MSU) is an volunteer, patient lead, patient-centered 501(c)(3) nonprofit organization dedicated to improving the lives of Myositis patients and caregivers. MSU was founded by Myositis patients and is Empowering the Myositis Community through education, clinical trial matching, support, advocacy, and financial assistance.
Learn more about MSU and get involved.
Get Support!
Myositis patients and care partners, connect free and anonymously with others who understand because they are going through the same or similar experiences. Get the caring, educational support you deserve by joining the Myositis Support Community, a partnership with Inspire, using the iOS app, or by visiting the Myositis Support Community website.
Simply Put
“Simply Put” is a service of Myositis Support and Understanding, to provide overviews of Myositis-related medical and scientific information in understandable language.
MSU volunteers, who have no medical background, read and analyze often-complicated medical information and present it in more simplified terms so that readers have a starting point for further investigation and consultation with healthcare providers. The information provided is not meant to be medical advice of any type.
The above information is provided as a basic overview of a complicated group of diseases. For more in-depth information, you are encouraged to explore the individual topics covered in the MSU website.